Indications and Usage
CADUET (amlodipine and atorvastatin) is indicated in patients for whom treatment with both amlodipine and atorvastatin is appropriate.
Amlodipine1.
Hypertension:Amlodipine is indicated for the treatment of hypertension. It may be used alone or in combination with other antihypertensive agents; 2.
Coronary Artery Disease (CAD)Chronic Stable Angina:
Amlodipine is indicated for the treatment of chronic stable angina. Amlodipine may be used alone or in combination with other antianginal or antihypertensive agents;
Vasospastic Angina (Prinzmetal's or Variant Angina):
Amlodipine is indicated for the treatment of confirmed or suspected vasospastic angina. Amlodipine may be used as monotherapy or in combination with other antianginal drugs.
Angiographically Documented CAD:
In patients with recently documented CAD by angiography and without heart failure or an ejection fraction less than 40%, amlodipine is indicated to reduce the risk of hospitalization due to angina and to reduce the risk of a coronary revascularization procedure.
AND
Atorvastatin
Therapy with lipid-altering agents should be only one component of multiple risk factor intervention in individuals at significantly increased risk for atherosclerotic vascular disease due to hypercholesterolemia. Drug therapy is recommended as an adjunct to diet when the response to a diet restricted in saturated fat and cholesterol and other nonpharmacologic measures alone has been inadequate. In patients with CHD or multiple risk factors for CHD, the atorvastatin component of CADUET can be started simultaneously with diet restriction.
1.
Prevention of Cardiovascular Disease:In adult patients without clinically evident coronary heart disease, but with multiple risk factors for coronary heart disease such as age, smoking, hypertension, low HDL-C, or a family history of early coronary heart disease, atorvastatin is indicated to:
- Reduce the risk of myocardial infarction
- Reduce the risk of stroke
- Reduce the risk for revascularization procedures and angina
In patients with type 2 diabetes, and without clinically evident coronary heart disease, but with multiple risk factors for coronary heart disease such as retinopathy, albuminuria, smoking, or hypertension, LIPITOR is indicated to:
- Reduce the risk of myocardial infarction
- Reduce the risk of stroke;
In patients with clinically evident coronary heart disease, LIPITOR is indicated to:
- Reduce the risk of non-fatal myocardial infarction
- Reduce the risk of fatal and non-fatal stroke
- Reduce the risk for revascularization procedures
- Reduce the risk of hospitalization for CHF
- Reduce the risk of angina
2.
Heterozygous Familial and Nonfamilial Hyperlipidemia:Atorvastatin is indicated as an adjunct to diet to reduce elevated total-C, LDL-C, apo B, and TG levels and to increase HDL-C in patients with primary hypercholesterolemia (heterozygous familial and nonfamilial) and mixed dyslipidemia (
FredricksonTypes IIa and IIb); 3.
Elevated Serum TG Levels:Atorvastatin is indicated as an adjunct to diet for the treatment of patients with elevated serum TG levels (
FredricksonType IV); 4.
Primary Dysbetalipoproteinemia:Atorvastatin is indicated for the treatment of patients with primary dysbetalipoproteinemia (
FredricksonType III) who do not respond adequately to diet; 5.
Homozygous Familial Hypercholesterolemia:Atorvastatin is indicated to reduce total-C and LDL-C in patients with homozygous familial hypercholesterolemia as an adjunct to other lipid-lowering treatments (e.g., LDL apheresis) or if such treatments are unavailable; 6.
Pediatric Patients:Atorvastatin is indicated as an adjunct to diet to reduce total-C, LDL-C, and apo B levels in boys and postmenarchal girls, 10 to 17 years of age, with heterozygous familial hypercholesterolemia if after an adequate trial of diet therapy the following findings are present:
- LDL-C remains greater than or equal to 190 mg/dL or
- LDL-C remains greater than or equal to 160 mg/dL and: there is a positive family history of premature cardiovascular disease or two or more other CVD risk factors are present in the pediatric patients.
The antidyslipidemic component of CADUET has not been studied in conditions where the major lipoprotein abnormality is elevation of chylomicrons (Fredrickson Types I and V).
Dosage and Administration
Dosage of CADUET must be individualized on the basis of both effectiveness and tolerance for each individual component in the treatment of hypertension/angina and hyperlipidemia.
Amlodipine (Hypertension or angina)
Adults
The usual initial antihypertensive oral dose of amlodipine is 5 mg once daily with a maximum dose of 10 mg once daily. Small, fragile, or elderly individuals, or patients with hepatic insufficiency may be started on 2.5 mg once daily and this dose may be used when adding amlodipine to other antihypertensive therapy.
Dosage should be adjusted according to each patient's need. In general, titration should proceed over 7 to 14 days so that the physician can fully assess the patient's response to each dose level. Titration may proceed more rapidly, however, if clinically warranted, provided the patient is assessed frequently.
The recommended dose of amlodipine for chronic stable or vasospastic angina is 5–10 mg, with the lower dose suggested in the elderly and in patients with hepatic insufficiency. Most patients will require 10 mg for adequate effect. See ADVERSE REACTIONS section for information related to dosage and side effects.
The recommended dose range of amlodipine for patients with coronary artery disease is 5–10 mg once daily. In clinical studies the majority of patients required 10 mg (see CLINICAL PHARMACOLOGY, Clinical studies ).
Children
The effective antihypertensive oral dose of amlodipine in pediatric patients ages 6–17 years is 2.5 mg to 5 mg once daily. Doses in excess of 5 mg daily have not been studied in pediatric patients (see CLINICAL PHARMACOLOGY ).
Atorvastatin (Hyperlipidemia)
Hyperlipidemia (Heterozygous Familial and Nonfamilial) and Mixed Dyslipidemia (Fredrickson Types IIa and IIb)
The recommended starting dose of atorvastatin is 10 or 20 mg once daily. Patients who require a large reduction in LDL-C (more than 45%) may be started at 40 mg once daily. The dosage range of atorvastatin is 10 to 80 mg once daily. Atorvastatin can be administered as a single dose at any time of the day, with or without food. The starting dose and maintenance doses of atorvastatin should be individualized according to patient characteristics such as goal of therapy and response (see current NCEP Guidelines). After initiation and/or upon titration of atorvastatin, lipid levels should be analyzed within 2 to 4 weeks and dosage adjusted accordingly.
Heterozygous Familial Hypercholesterolemia in Pediatric Patients (10–17 years of age)
The recommended starting dose of atorvastatin is 10 mg/day; the maximum recommended dose is 20 mg/day (doses greater than 20 mg have not been studied in this patient population). Doses should be individualized according to the recommended goal of therapy (see current NCEP Pediatric Panel Guidelines3, CLINICAL PHARMACOLOGY , and INDICATIONS AND USAGE ). Adjustments should be made at intervals of 4 weeks or more.
3National Cholesterol Education Program (NCEP): Highlights of the Report of the Expert Panel on Blood Cholesterol Levels in Children Adolescents.
Pediatrics. 89(3):495–501. 1992.
Homozygous Familial Hypercholesterolemia
The dosage of atorvastatin in patients with homozygous FH is 10 to 80 mg daily. Atorvastatin should be used as an adjunct to other lipid-lowering treatments (e.g., LDL apheresis) in these patients or if such treatments are unavailable. Note: a 2.5/80 mg CADUET tablet is not available. Management of patients needing a 2.5/80 mg combination requires individual assessments of dyslipidemia and therapy with the individual components as a 2.5/80 mg CADUET tablet is not available.
Concomitant Lipid Lowering Therapy
Atorvastatin may be used with bile acid resins. Monitor for signs of myopathy in patients receiving the combination of statins and fibrates (see WARNINGS, Skeletal Muscle , and PRECAUTIONS, Drug Interactions ).
Dosage in Patients With Renal Impairment
Renal disease does not affect the plasma concentrations nor LDL-C reduction of atorvastatin; thus, dosage adjustment in patients with renal dysfunction is not necessary (see WARNINGS, Skeletal Muscle , and CLINICAL PHARMACOLOGY, Specific Populations ).
Dosage in Patients Taking Cyclosporine, Clarithromycin, Itraconazole, or a Combination of Ritonavir plus Saquinavir or Lopinavir plus Ritonavir
In patients taking cyclosporine, therapy should be limited to LIPITOR 10 mg once daily. In patients taking clarithromycin, itraconazole or in patients with HIV taking a combination of ritonavir plus saquinavir or lopinavir plus ritonavir, for doses of atorvastatin exceeding 20 mg, appropriate clinical assessment is recommended to ensure that the lowest dose necessary of atorvastatin is employed (see WARNINGS, Skeletal Muscle , and PRECAUTIONS, Drug Interactions ).
CADUET
CADUET may be substituted for its individually titrated components. Patients may be given the equivalent dose of CADUET or a dose of CADUET with increased amounts of amlodipine, atorvastatin or both for additional antianginal effects, blood pressure lowering, or lipid lowering effect.
CADUET may be used to provide additional therapy for patients already on one of its components. As initial therapy for one indication and continuation of treatment of the other, the recommended starting dose of CADUET should be selected based on the continuation of the component being used and the recommended starting dose for the added monotherapy.
CADUET may be used to initiate treatment in patients with hyperlipidemia and either hypertension or angina. The recommended starting dose of CADUET should be based on the appropriate combination of recommendations for the monotherapies. The maximum dose of the amlodipine component of CADUET is 10 mg once daily. The maximum dose of the atorvastatin component of CADUET is 80 mg once daily.
See above for detailed information related to the dosing and administration of amlodipine and atorvastatin.
Contraindications
CADUET contains atorvastatin and is therefore contraindicated in patients with active liver disease, which may include unexplained persistent elevations in hepatic transaminase levels.
CADUET is contraindicated in patients with known hypersensitivity to any component of this medication.
Pregnancy and Lactation
CADUET contains atorvastatin and is therefore contraindicated in women who are pregnant or may become pregnant. The atorvastatin component of CADUET may cause fetal harm when administered to a pregnant woman. Serum cholesterol and triglycerides increase during normal pregnancy, and cholesterol or cholesterol derivatives are essential for fetal development. Atherosclerosis is a chronic process and discontinuation of lipid-lowering drugs during pregnancy should have little impact on the outcome of long-term therapy of primary hypercholesterolemia.
There are no adequate and well-controlled studies of atorvastatin use during pregnancy; however in rare reports congenital anomalies were observed following intrauterine exposure to statins. In rat and rabbit animal reproduction studies, atorvastatin revealed no evidence of teratogenicity. CADUET, WHICH INCLUDES ATORVASTATIN, SHOULD BE ADMINISTERED TO WOMEN OF CHILDBEARING AGE ONLY WHEN SUCH PATIENTS ARE HIGHLY UNLIKELY TO CONCEIVE AND HAVE BEEN INFORMED OF THE POTENTIAL HAZARDS. If the patient becomes pregnant while taking this drug, therapy should be discontinued immediately and the patient apprised of the potential hazard to the fetus (see PRECAUTIONS, Pregnancy ).
It is not known whether atorvastatin or amlodipine are excreted into human milk; however a small amount of another statin does pass into breast milk. Because statins have the potential for serious adverse reactions in nursing infants, women taking CADUET should not breastfeed their infants (see PRECAUTIONS, Nursing Mothers ).
Adverse Reactions
CADUET
CADUET (amlodipine besylate/atorvastatin calcium) has been evaluated for safety in 1092 patients in double-blind placebo controlled studies treated for co-morbid hypertension and dyslipidemia. In general, treatment with CADUET was well tolerated. For the most part, adverse experiences have been mild or moderate in severity. In clinical trials with CADUET, no adverse experiences peculiar to this combination have been observed. Adverse experiences are similar in terms of nature, severity, and frequency to those reported previously with amlodipine and atorvastatin.
The following information is based on the clinical experience with amlodipine and atorvastatin.
The Amlodipine Component of CADUET
Amlodipine has been evaluated for safety in more than 11,000 patients in U.S. and foreign clinical trials. In general, treatment with amlodipine was well tolerated at doses up to 10 mg daily. Most adverse reactions reported during therapy with amlodipine were of mild or moderate severity. In controlled clinical trials directly comparing amlodipine (N=1730) in doses up to 10 mg to placebo (N=1250), discontinuation of amlodipine due to adverse reactions was required in only about 1.5% of patients and was not significantly different from placebo (about 1%). The most common side effects are headache and edema. The incidence (%) of side effects which occurred in a dose related manner are as follows:
| Adverse Event | amlodipine | |||
|---|---|---|---|---|
|
|
2.5 mg N=275 |
5.0 mg N=296 |
10.0 mg N=268 |
Placebo N=520 |
| Edema | 1.8 | 3.0 | 10.8 | 0.6 |
| Dizziness | 1.1 | 3.4 | 3.4 | 1.5 |
| Flushing | 0.7 | 1.4 | 2.6 | 0.0 |
| Palpitations | 0.7 | 1.4 | 4.5 | 0.6 |
Other adverse experiences which were not clearly dose related but which were reported with an incidence greater than 1.0% in placebo-controlled clinical trials include the following:
Placebo-Controlled Studies
| Adverse Event | amlodipine (%) (N=1730) |
Placebo (%) (N=1250) |
|---|---|---|
| Headache | 7.3 | 7.8 |
| Fatigue | 4.5 | 2.8 |
| Nausea | 2.9 | 1.9 |
| Abdominal Pain | 1.6 | 0.3 |
| Somnolence | 1.4 | 0.6 |
For several adverse experiences that appear to be drug and dose related, there was a greater incidence in women than men associated with amlodipine treatment as shown in the following table:
| Adverse Event | amlodipine | Placebo | ||
|---|---|---|---|---|
|
|
M=% (N=1218) |
F=% (N=512) |
M=% (N=914) |
F=% (N=336) |
| Edema | 5.6 | 14.6 | 1.4 | 5.1 |
| Flushing | 1.5 | 4.5 | 0.3 | 0.9 |
| Palpitations | 1.4 | 3.3 | 0.9 | 0.9 |
| Somnolence | 1.3 | 1.6 | 0.8 | 0.3 |
The following events occurred in ≤1% but >0.1% of patients treated with amlodipine in controlled clinical trials or under conditions of open trials or marketing experience where a causal relationship is uncertain; they are listed to alert the physician to a possible relationship:
Cardiovascular: arrhythmia (including ventricular tachycardia and atrial fibrillation), bradycardia, chest pain, hypotension, peripheral ischemia, syncope, tachycardia, postural dizziness, postural hypotension, vasculitis.
Central and Peripheral Nervous System: hypoesthesia, neuropathy peripheral, paresthesia, tremor, vertigo.
Gastrointestinal: anorexia, constipation, dyspepsia,2 dysphagia, diarrhea, flatulence, pancreatitis, vomiting, gingival hyperplasia.
General: allergic reaction, asthenia,2 back pain, hot flushes, malaise, pain, rigors, weight gain, weight decrease.
Musculoskeletal System: arthralgia, arthrosis, muscle cramps,2 myalgia.
Psychiatric: sexual dysfunction (male2 and female), insomnia, nervousness, depression, abnormal dreams, anxiety, depersonalization.
Respiratory System: dyspnea,2 epistaxis.
Skin and Appendages: angioedema, erythema multiforme, pruritus,2 rash,2 rash erythematous, rash maculopapular.
Special Senses: abnormal vision, conjunctivitis, diplopia, eye pain, tinnitus.
Urinary System: micturition frequency, micturition disorder, nocturia.
Autonomic Nervous System: dry mouth, sweating increased.
Metabolic and Nutritional: hyperglycemia, thirst.
Hemopoietic: leukopenia, purpura, thrombocytopenia.
The following events occurred in ≤0.1% of patients treated with amlodipine in controlled clinical trials or under conditions of open trials or marketing experience: cardiac failure, pulse irregularity, extrasystoles, skin discoloration, urticaria, skin dryness, alopecia, dermatitis, muscle weakness, twitching, ataxia, hypertonia, migraine, cold and clammy skin, apathy, agitation, amnesia, gastritis, increased appetite, loose stools, coughing, rhinitis, dysuria, polyuria, parosmia, taste perversion, abnormal visual accommodation, and xerophthalmia.
Other reactions occurred sporadically and cannot be distinguished from medications or concurrent disease states such as myocardial infarction and angina.
Amlodipine therapy has not been associated with clinically significant changes in routine laboratory tests. No clinically relevant changes were noted in serum potassium, serum glucose, total triglycerides, total cholesterol, HDL cholesterol, uric acid, blood urea nitrogen, or creatinine.
In the CAMELOT and PREVENT studies (see CLINICAL PHARMACOLOGY Clinical Studies, Clinical Studies with Amlodipine ) the adverse event profile was similar to that reported previously (see above), with the most common adverse event being peripheral edema.
The following postmarketing event has been reported infrequently with amlodipine treatment where a causal relationship is uncertain: gynecomastia. In postmarketing experience, jaundice and hepatic enzyme elevations (mostly consistent with cholestasis or hepatitis) in some cases severe enough to require hospitalization have been reported in association with use of amlodipine.
Amlodipine has been used safely in patients with chronic obstructive pulmonary disease, well-compensated congestive heart failure, peripheral vascular disease, diabetes mellitus, and abnormal lipid profiles.
2These events occurred in less than 1% in placebo-controlled trials, but the incidence of these side effects was between 1% and 2% in all multiple dose studies.
The Atorvastatin Component of CADUET
The following serious adverse reactions are discussed in greater
detail in other sections of the label:
Rhabdomyolysis and myopathy (see
WARNINGS, Skeletal
Muscle
)
Liver enzyme abnormalities (see
WARNINGS, Liver Dysfunction
)
Clinical Adverse Experiences
Because clinical trials are conducted under widely varying conditions, the adverse reaction rates observed in the clinical studies of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
In the LIPITOR placebo-controlled clinical trial database of 16,066 patients (8755 LIPITOR vs. 7311 placebo; age range 10–93 years, 39% women, 91% Caucasians, 3% Blacks, 2% Asians, 4% other) with a median treatment duration of 53 weeks, 9.7% of patients on LIPITOR and 9.5% of the patients on placebo discontinued due to adverse reactions regardless of causality. The five most common adverse reactions in patients treated with LIPITOR that led to treatment discontinuation and occurred at a rate greater than placebo were: myalgia (0.7%), diarrhea (0.5%), nausea (0.4%), alanine aminotransferase increase (0.4%), and hepatic enzyme increase (0.4%).
The most commonly reported adverse reactions (incidence ≥ 2% and greater than placebo) regardless of causality, in patients treated with LIPITOR in placebo controlled trials (n=8755) were: nasopharyngitis (8.3%), arthralgia (6.9%), diarrhea (6.8%), pain in extremity (6.0%), and urinary tract infection (5.7%).
Table 13 summarizes the frequency of clinical adverse reactions, regardless of causality, reported in ≥ 2% and at a rate greater than placebo in patients treated with LIPITOR (n=8755), from seventeen placebo-controlled trials.
| Adverse Reaction * |
Any dose N=8755 |
10 mg N=3908 |
20 mg N=188 |
40 mg N=604 |
80 mg N=4055 |
Placebo N=7311 |
| Nasopharyngitis |
8.3 |
12.9 |
5.3 |
7.0 |
4.2 |
8.2 |
| Arthralgia |
6.9 |
8.9 |
11.7 |
10.6 |
4.3 |
6.5 |
| Diarrhea |
6.8 |
7.3 |
6.4 |
14.1 |
5.2 |
6.3 |
| Pain in extremity |
6.0 |
8.5 |
3.7 |
9.3 |
3.1 |
5.9 |
| Urinary tract infection |
5.7 |
6.9 |
6.4 |
8.0 |
4.1 |
5.6 |
| Dyspepsia |
4.7 |
5.9 |
3.2 |
6.0 |
3.3 |
4.3 |
| Nausea |
4.0 |
3.7 |
3.7 |
7.1 |
3.8 |
3.5 |
| Musculoskeletal pain |
3.8 |
5.2 |
3.2 |
5.1 |
2.3 |
3.6 |
| Muscle Spasm |
3.6 |
4.6 |
4.8 |
5.1 |
2.4 |
3.0 |
| Myalgia |
3.5 |
3.6 |
5.9 |
8.4 |
2.7 |
3.1 |
| Insomnia |
3.0 |
2.8 |
1.1 |
5.3 |
2.8 |
2.9 |
| Pharyngolaryngeal pain |
2.3 |
3.9 |
1.6 |
2.8 |
0.7 |
2.1 |
Adverse Reaction greater than or equal to 2% in any dose greater than placebo
Other adverse reactions reported in placebo-controlled studies
include:
Body as a whole: malaise, pyrexia; Digestive system: abdominal discomfort, eructation,
flatulence, hepatitis, cholestasis; Musculoskeletal
system: musculoskeletal pain, muscle fatigue, neck pain, joint swelling;
Metabolic and nutritional system: transaminases
increase, liver function test abnormal, blood alkaline phosphatase increase,
creatine phosphokinase increase, hyperglycemia; Nervous
system: nightmare; Respiratory system:
epistaxis; Skin and appendages: urticaria; Special senses: vision blurred, tinnitus; Urogenital system: white blood cells urine positive.
Anglo-Scandinavian Cardiac Outcomes Trial (ASCOT)
In ASCOT (see CLINICAL PHARMACOLOGY, Clinical Studies, Clinical Studies with Atorvastatin ) involving 10,305 participants (age range 40–80 years, 19% women; 94.6% Caucasians, 2.6% Africans, 1.5% South Asians, 1.3% mixed/other) treated with atorvastatin 10 mg daily (n=5,168) or placebo (n=5,137), the safety and tolerability profile of the group treated with atorvastatin was comparable to that of the group treated with placebo during a median of 3.3 years of follow-up.
Collaborative Atorvastatin Diabetes Study (CARDS)
In CARDS (see CLINICAL PHARMACOLOGY, Clinical Studies, Clinical Studies with Atorvastatin ) involving 2838 subjects (age range 39–77 years, 32% women; 94.3% Caucasians, 2.4% South Asians, 2.3% Afro-Caribbean, 1.0% other)with type 2 diabetes treated with LIPITOR 10 mg daily (n=1428) or placebo (n=1410), there was no difference in the overall frequency of adverse reactions or serious adverse reactions between the treatment groups during a median follow-up of 3.9 years. No cases of rhabdomyolysis were reported.
Treating to New Targets Study (TNT)
In TNT (see CLINICAL PHARMACOLOGY, Clinical Studies ) involving 10,001 subjects (age range 29–78 years, 19% women; 94.1% Caucasians, 2.9% Blacks, 1.0% Asians, 2.0% other) with clinically evident CHD treated with LIPITOR 10 mg daily (n=5006) or LIPITOR 80 mg daily (n=4995), there were more serious adverse reactions and discontinuations due to adverse reactions in the high-dose atorvastatin group (92, 1.8%; 497, 9.9%, respectively) as compared to the low-dose group (69, 1.4%; 404, 8.1%, respectively) during a median follow-up of 4.9 years. Persistent transaminase elevations (≥3 × ULN twice within 4–10 days) occurred in 62 (1.3%) individuals with atorvastatin 80 mg and in nine (0.2%) individuals with atorvastatin 10 mg. Elevations of CK (≥ 10 × ULN) were low overall, but were higher in the high-dose atorvastatin treatment group (13, 0.3%) compared to the low-dose atorvastatin group (6, 0.1%).
Incremental Decrease in Endpoints Through Aggressive Lipid Lowering Study (IDEAL)
In IDEAL (see CLINICAL PHARMACOLOGY, Clinical Studies ) involving 8,888 subjects (age range 26–80 years, 19% women; 99.3% Caucasians, 0.4% Asians, 0.3% Blacks, 0.04% other) treated with LIPITOR 80 mg/day (n=4439) or simvastatin 20–40 mg daily (n=4449), there was no difference in the overall frequency of adverse reactions or serious adverse reactions between the treatment groups during a median follow-up of 4.8 years.
Stroke Prevention by Aggressive Reduction in Cholesterol Levels (SPARCL)
In SPARCL involving 4731 subjects (age range 21–92 years, 40% women; 93.3% Caucasians, 3.0% Blacks, 0.6% Asians, 3.1% other) without clinically evident CHD but with a stroke or transient ischemic attack (TIA) within the previous 6 months treated with LIPITOR 80 mg (n=2365) or placebo (n=2366) for a median follow-up of 4.9 years, there was a higher incidence of persistent hepatic transaminase elevations (≥ 3 × ULN twice within 4–10 days) in the atorvastatin group (0.9%) compared to placebo (0.1%). Elevations of CK (>10 × ULN) were rare, but were higher in the atorvastatin group (0.1%) compared to placebo (0.0%). Diabetes was reported as an adverse reaction in 144 subjects (6.1%) in the atorvastatin group and 89 subjects (3.8%) in the placebo group (see PRECAUTIONS ).
In a post-hoc analysis, LIPITOR 80 mg reduced the incidence of ischemic stroke (218/2365, 9.2% vs. 274/2366, 11.6%) and increased the incidence of hemorrhagic stroke (55/2365, 2.3% vs. 33/2366, 1.4%) compared to placebo. The incidence of fatal hemorrhagic stroke was similar between groups (17 LIPITOR vs. 18 placebo). The incidence of non-fatal hemorrhagic strokes was significantly greater in the atorvastatin group (38 non-fatal hemorrhagic strokes) as compared to the placebo group (16 non-fatal hemorrhagic strokes). Subjects who entered the study with a hemorrhagic stroke appeared to be at increased risk for hemorrhagic stroke [7 (16%) LIPITOR vs. 2 (4%) placebo].
There were no significant differences between the treatment groups for all-cause mortality: 216 (9.1%) in the LIPITOR 80 mg/day group vs. 211 (8.9%) in the placebo group. The proportions of subjects who experienced cardiovascular death were numerically smaller in the LIPITOR 80 mg group (3.3%) than in the placebo group (4.1%). The proportions of subjects who experienced non-cardiovascular death were numerically larger in the LIPITOR 80 mg group (5.0%) than in the placebo group (4.0%).
Postintroduction Reports with Atorvastatin
The following adverse reactions have been identified during postapproval use of the atorvastatin component of CADUET. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Adverse reactions associated with atorvastatin therapy reported since market introduction, that are not listed above, regardless of causality assessment, include the following: anaphylaxis, angioneurotic edema, bullous rashes (including erythema multiforme, Stevens-Johnson syndrome, and toxic epidermal necrolysis), rhabdomyolysis, fatigue, tendon rupture, hepatic failure, dizziness, memory impairment, depression, and peripheral neuropathy.
Pediatric Patients (ages 10–17 years)
In a 26-week controlled study in boys and postmenarchal girls (n=140, 31% female; 92% Caucasians, 1.6% Blacks, 1.6% Asians, 4.8% other), the safety and tolerability profile of atorvastatin 10 to 20 mg daily was generally similar to that of placebo (see CLINICAL PHARMACOLOGY, Clinical Studies section and PRECAUTIONS, Pediatric Use ).
Overdosage
There is no information on overdosage with CADUET in humans.
Information on Amlodipine
Single oral doses of amlodipine maleate equivalent to 40 mg amlodipine/kg and 100 mg amlodipine/kg in mice and rats, respectively, caused deaths. Single oral amlodipine maleate doses equivalent to 4 or more mg amlodipine/kg in dogs (11 or more times the maximum recommended clinical dose on a mg/m2 basis) caused a marked peripheral vasodilation and hypotension.
Overdosage might be expected to cause excessive peripheral vasodilation with marked hypotension and possibly a reflex tachycardia. In humans, experience with intentional overdosage of amlodipine is limited. Reports of intentional overdosage include a patient who ingested 250 mg and was asymptomatic and was not hospitalized; another (120 mg) was hospitalized, underwent gastric lavage and remained normotensive; the third (105 mg) was hospitalized and had hypotension (90/50 mmHg) which normalized following plasma expansion. A patient who took 70 mg amlodipine and an unknown quantity of benzodiazepine in a suicide attempt developed shock which was refractory to treatment and died the following day with abnormally high benzodiazepine plasma concentration. A case of accidental drug overdose has been documented in a 19-month-old male who ingested 30 mg amlodipine (about 2 mg/kg). During the emergency room presentation, vital signs were stable with no evidence of hypotension, but a heart rate of 180 bpm. Ipecac was administered 3.5 hours after ingestion and on subsequent observation (overnight) no sequelae were noted.
If overdose should occur, begin active cardiac and respiratory monitoring. Perform frequent blood pressure measurements. Should hypotension occur, initiate cardiovascular support including elevation of the extremities and administration of fluids. If hypotension remains unresponsive to these conservative measures, consider administration of vasopressors (such as phenylephrine) with specific attention to circulating volume and urine output. As amlodipine is highly protein bound, hemodialysis is not likely to be of benefit.
Information on Atorvastatin
There is no specific treatment for atorvastatin overdosage. In the event of an overdose, the patient should be treated symptomatically, and supportive measures instituted as required. Due to extensive drug binding to plasma proteins, hemodialysis is not expected to significantly enhance atorvastatin clearance.
Description
CADUET® (amlodipine besylate and atorvastatin calcium) tablets combine the calcium channel blocker amlodipine besylate with the lipid-lowering agent atorvastatin calcium.
The amlodipine besylate component of CADUET is chemically described as 3-ethyl-5-methyl (±)-2-[(2-aminoethoxy)methyl]-4-(o-chlorophenyl)-1,4-dihydro-6-methyl-3,5-pyridinedicarboxylate, monobenzenesulphonate. Its empirical formula is C20H25ClN2O5•C6H6O3S.
The atorvastatin calcium component of CADUET is chemically described as [R-(R*, R*)]-2-(4-fluorophenyl)-β, δ-dihydroxy-5-(1-methylethyl)-3-phenyl-4-[(phenylamino)carbonyl]-1H-pyrrole-1-heptanoic acid, calcium salt (2:1) trihydrate. Its empirical formula is (C33H34FN2O5)2Ca•3H2O.
The structural formulae for amlodipine besylate and atorvastatin calcium are shown below.
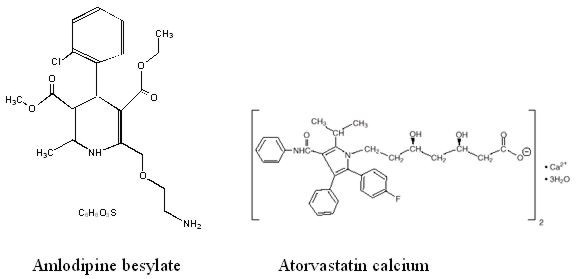
CADUET contains amlodipine besylate, a white to off-white crystalline powder, and atorvastatin calcium, also a white to off-white crystalline powder. Amlodipine besylate has a molecular weight of 567.1 and atorvastatin calcium has a molecular weight of 1209.42. Amlodipine besylate is slightly soluble in water and sparingly soluble in ethanol. Atorvastatin calcium is insoluble in aqueous solutions of pH 4 and below. Atorvastatin calcium is very slightly soluble in distilled water, pH 7.4 phosphate buffer, and acetonitrile; slightly soluble in ethanol, and freely soluble in methanol.
CADUET tablets are formulated for oral administration in the following strength combinations:
|
|
2.5 mg/ 10mg |
2.5 mg/ 20mg |
2.5 mg/ 40mg |
5 mg/10 mg |
5 mg/20 mg |
5 mg/40 mg |
5 mg/80 mg |
10 mg/ 10 mg |
10 mg/ 20 mg |
10 mg/ 40 mg |
10 mg/ 80 mg |
|---|---|---|---|---|---|---|---|---|---|---|---|
| amlodipine equivalent (mg) |
2.5 | 2.5 | 2.5 | 5 | 5 | 5 | 5 | 10 | 10 | 10 | 10 |
| atorvastatin equivalent (mg) |
10 | 20 | 40 | 10 | 20 | 40 | 80 | 10 | 20 | 40 | 80 |
Each tablet also contains calcium carbonate, croscarmellose sodium, microcrystalline cellulose, pregelatinized starch, polysorbate 80, hydroxypropyl cellulose, purified water, colloidal silicon dioxide (anhydrous), magnesium stearate, Opadry® II White 85F28751 (polyvinyl alcohol, titanium dioxide, PEG 3000 and talc) or Opadry® II Blue 85F10919 (polyvinyl alcohol, titanium dioxide, PEG 3000, talc and FD&C blue #2). Combinations of atorvastatin with 2.5 mg and 5 mg amlodipine are film coated white, and combinations of atorvastatin with 10 mg amlodipine are film coated blue.
image of both chemical structuresClinical Pharmacology
Mechanism of Action
CADUET
CADUET is a combination of two drugs, a dihydropyridine calcium channel blocker amlodipine and an HMG-CoA reductase inhibitor atorvastatin. The amlodipine component of CADUET inhibits the transmembrane influx of calcium ions into vascular smooth muscle and cardiac muscle. The atorvastatin component of CADUET is a selective, competitive inhibitor of HMG-CoA reductase (statin), the rate-limiting enzyme that converts 3-hydroxy-3-methylglutaryl-coenzyme A to mevalonate, a precursor of sterols, including cholesterol.
Amlodipine
Experimental data suggest that amlodipine binds to both dihydropyridine and nondihydropyridine binding sites. The contractile processes of cardiac muscle and vascular smooth muscle are dependent upon the movement of extracellular calcium ions into these cells through specific ion channels. Amlodipine inhibits calcium ion influx across cell membranes selectively, with a greater effect on vascular smooth muscle cells than on cardiac muscle cells. Negative inotropic effects can be detected in vitro but such effects have not been seen in intact animals at therapeutic doses. Serum calcium concentration is not affected by amlodipine.
Amlodipine is a peripheral arterial vasodilator that acts directly on vascular smooth muscle to cause a reduction in peripheral vascular resistance and reduction in blood pressure.
The precise mechanisms by which amlodipine relieves angina have not been fully delineated, but are thought to include the following:
Exertional Angina: In patients with exertional angina, amlodipine reduces the total peripheral resistance (afterload) against which the heart works and reduces the rate pressure product, and thus myocardial oxygen demand, at any given level of exercise.
Vasospastic Angina: Amlodipine has been demonstrated to block constriction and restore blood flow in coronary arteries and arterioles in response to calcium, potassium epinephrine, serotonin, and thromboxane A2 analog in experimental animal models and in human coronary vessels in vitro. This inhibition of coronary spasm is responsible for the effectiveness of amlodipine in vasospastic (Prinzmetal's or variant) angina.
Atorvastatin
Cholesterol and triglycerides circulate in the bloodstream as part of lipoprotein complexes. With ultracentrifugation, these complexes separate into HDL (high-density lipoprotein), IDL (intermediate-density lipoprotein), LDL (low-density lipoprotein), and VLDL (very-low-density lipoprotein) fractions. Triglycerides (TG) and cholesterol in the liver are incorporated into VLDL and released into the plasma for delivery to peripheral tissues. LDL is formed from VLDL and is catabolized primarily through the high-affinity LDL receptor.
Clinical and pathologic studies show that elevated plasma levels of total cholesterol (total-C), LDL-cholesterol (LDL-C), and apolipoprotein B (apo B) promote human atherosclerosis and are risk factors for developing cardiovascular disease, while increased levels of HDL-C are associated with a decreased cardiovascular risk.
Epidemiologic investigations have established that cardiovascular morbidity and mortality vary directly with the level of total-C and LDL-C, and inversely with the level of HDL-C.
In animal models, atorvastatin lowers plasma cholesterol and lipoprotein levels by inhibiting HMG-CoA reductase and cholesterol synthesis in the liver and by increasing the number of hepatic LDL receptors on the cell-surface to enhance uptake and catabolism of LDL; atorvastatin also reduces LDL production and the number of LDL particles.
Atorvastatin reduces total-C, LDL-C, and apo B in patients with homozygous and heterozygous familial hypercholesterolemia (FH), nonfamilial forms of hypercholesterolemia, and mixed dyslipidemia. Atorvastatin also reduces VLDL-C and TG and produces variable increases in HDL-C and apolipoprotein A-1. Atorvastatin reduces total-C, LDL-C, VLDL-C, apo B, TG, and non-HDL-C, and increases HDL-C in patients with isolated hypertriglyceridemia. Atorvastatin reduces intermediate density lipoprotein cholesterol (IDL-C) in patients with dysbetalipoproteinemia.
Like LDL, cholesterol-enriched triglyceride-rich lipoproteins, including VLDL, intermediate density lipoprotein (IDL), and remnants, can also promote atherosclerosis. Elevated plasma triglycerides are frequently found in a triad with low HDL-C levels and small LDL particles, as well as in association with non-lipid metabolic risk factors for coronary heart disease. As such, total plasma TG has not consistently been shown to be an independent risk factor for CHD. Furthermore, the independent effect of raising HDL or lowering TG on the risk of coronary and cardiovascular morbidity and mortality has not been determined.
Pharmacokinetics and Metabolism
Absorption
Studies with amlodipine
After oral administration of therapeutic doses of amlodipine alone, absorption produces peak plasma concentrations between 6 and 12 hours. Absolute bioavailability has been estimated to be between 64% and 90%.
Studies with atorvastatin
After oral administration alone, atorvastatin is rapidly absorbed; maximum plasma concentrations occur within 1 to 2 hours. Extent of absorption increases in proportion to atorvastatin dose. The absolute bioavailability of atorvastatin (parent drug) is approximately 14% and the systemic availability of HMG-CoA reductase inhibitory activity is approximately 30%. The low systemic availability is attributed to presystemic clearance in gastrointestinal mucosa and/or hepatic first-pass metabolism. Plasma atorvastatin concentrations are lower (approximately 30% for Cmax and AUC) following evening drug administration compared with morning. However, LDL-C reduction is the same regardless of the time of day of drug administration (see DOSAGE AND ADMINISTRATION ).
Studies with CADUET
Following oral administration of CADUET peak plasma concentrations of amlodipine and atorvastatin are seen at 6 to 12 hours and 1 to 2 hours post dosing, respectively. The rate and extent of absorption (bioavailability) of amlodipine and atorvastatin from CADUET are not significantly different from the bioavailability of amlodipine and atorvastatin administered separately (see above).
The bioavailability of amlodipine from CADUET was not affected by food. Food decreases the rate and extent of absorption of atorvastatin from CADUET by approximately 32% and 11%, respectively, as it does with atorvastatin when given alone. LDL-C reduction is similar whether atorvastatin is given with or without food.
Distribution
Studies with amlodipine
Ex vivo studies have shown that approximately 93% of the circulating amlodipine drug is bound to plasma proteins in hypertensive patients. Steady-state plasma levels of amlodipine are reached after 7 to 8 days of consecutive daily dosing.
Studies with atorvastatin
Mean volume of distribution of atorvastatin is approximately 381 liters. Atorvastatin is ≥98% bound to plasma proteins. A blood/plasma ratio of approximately 0.25 indicates poor drug penetration into red blood cells. Based on observations in rats, atorvastatin calcium is likely to be secreted in human milk (see CONTRAINDICATIONS, Pregnancy and Lactation, and PRECAUTIONS, Nursing Mothers ).
Metabolism
Studies with amlodipine
Amlodipine is extensively (about 90%) converted to inactive metabolites via hepatic metabolism.
Studies with atorvastatin
Atorvastatin is extensively metabolized to ortho- and parahydroxylated derivatives and various beta-oxidation products. In vitro inhibition of HMG-CoA reductase by ortho- and parahydroxylated metabolites is equivalent to that of atorvastatin. Approximately 70% of circulating inhibitory activity for HMG-CoA reductase is attributed to active metabolites. In vitro studies suggest the importance of atorvastatin metabolism by cytochrome P450 3A4, consistent with increased plasma concentrations of atorvastatin in humans following coadministration with erythromycin, a known inhibitor of this isozyme (see PRECAUTIONS, Drug Interactions ). In animals, the ortho-hydroxy metabolite undergoes further glucuronidation.
Excretion
Studies with amlodipine
Elimination from the plasma is biphasic with a terminal elimination half-life of about 30–50 hours. Ten percent of the parent amlodipine compound and 60% of the metabolites of amlodipine are excreted in the urine.
Studies with atorvastatin
Atorvastatin and its metabolites are eliminated primarily in bile following hepatic and/or extra-hepatic metabolism; however, the drug does not appear to undergo enterohepatic recirculation. Mean plasma elimination half-life of atorvastatin in humans is approximately 14 hours, but the half-life of inhibitory activity for HMG-CoA reductase is 20 to 30 hours due to the contribution of active metabolites. Less than 2% of a dose of atorvastatin is recovered in urine following oral administration.
Specific Populations
Geriatric
Studies with amlodipine
Elderly patients have decreased clearance of amlodipine with a resulting increase in AUC of approximately 40–60%, and a lower initial dose of amlodipine may be required.
Studies with atorvastatin
Plasma concentrations of atorvastatin are higher (approximately 40% for Cmax and 30% for AUC) in healthy elderly subjects (age ≥65 years) than in young adults. Clinical data suggest a greater degree of LDL-lowering at any dose of atorvastatin in the elderly population compared to younger adults (see PRECAUTIONS , Geriatric Use ).
Pediatric
Studies with amlodipine
Sixty-two hypertensive patients aged 6 to 17 years received doses of amlodipine between 1.25 mg and 20 mg. Weight-adjusted clearance and volume of distribution were similar to values in adults.
Studies with atorvastatin
Pharmacokinetic data in the pediatric population are not available.
Gender
Studies with atorvastatin
Plasma concentrations of atorvastatin in women differ from those in men (approximately 20% higher for Cmax and 10% lower for AUC); however, there is no clinically significant difference in LDL-C reduction with atorvastatin between men and women.
Renal Impairment
Studies with amlodipine
The pharmacokinetics of amlodipine are not significantly influenced by renal impairment. Patients with renal failure may therefore receive the usual initial amlodipine dose.
Studies with atorvastatin
Renal disease has no influence on the plasma concentrations or LDL-C reduction of atorvastatin; thus, dose adjustment of atorvastatin in patients with renal dysfunction is not necessary (see DOSAGE AND ADMINISTRATION and WARNINGS, Skeletal Muscle ).
Hemodialysis
While studies have not been conducted in patients with end-stage renal disease, hemodialysis is not expected to clear atorvastatin or amlodipine since both drugs are extensively bound to plasma proteins.
Hepatic Impairment
Atorvastatin is contraindicated in patients with active liver disease.
Studies with amlodipine
Elderly patients and patients with hepatic insufficiency have decreased clearance of amlodipine with a resulting increase in AUC of approximately 40–60%.
Studies with atorvastatin
In patients with chronic alcoholic liver disease, plasma concentrations of atorvastatin are markedly increased. Cmax and AUC are each 4-fold greater in patients with Childs-Pugh A disease. Cmax and AUC of atorvastatin are approximately 16-fold and 11-fold increased, respectively, in patients with Childs-Pugh B disease (see CONTRAINDICATIONS ).
Heart Failure
Studies with amlodipine
In patients with moderate to severe heart failure, the increase in AUC for amlodipine was similar to that seen in the elderly and in patients with hepatic insufficiency.
Pharmacokinetic Studies of Atorvastatin and Co-Administered Drugs
|
Co-administered drug and dosing regimen
|
|
Atorvastatin
|
|
|
|
Dose (mg)
|
Change in AUC * | Change in Cmax * |
| †Cyclosporine 5.2 mg/kg/day, stable dose | 10 mg QD for 28 days |
↑ 8.7-fold | ↑ 10.7-fold |
| †Lopinavir 400 mg BID/ ritonavir 100 mg BID, 14 days | 20 mg QD for 4 days |
↑ 5.9-fold | ↑ 4.7-fold |
| †Ritonavir 400 mg BID/ saquinavir 400mg BID, 15 days | 40 mg QD for 4 days |
↑ 3.9-fold | ↑ 4.3-fold |
| †Clarithromycin 500 mg BID, 9 days | 80 mg QD for 8 days |
↑ 4.4-fold | ↑ 5.4-fold |
| †Itraconazole 200 mg QD, 4 days | 40 mg SD |
↑ 3.3-fold | ↑ 20% |
| †Grapefruit Juice, 240 mL QD ‡ | 40 mg, SD |
↑ 37% |
↑ 16% |
| Diltiazem 240 mg QD, 28 days |
40 mg, SD |
↑ 51% | No change |
| Erythromycin 500 mg QID, 7 days |
10 mg, SD |
↑ 33% | ↑ 38% |
| Amlodipine 10 mg, single dose |
80 mg, SD |
↑ 15% | ↓ 12% |
| Cimetidine 300 mg QD, 4 weeks |
10 mg QD for 2 weeks |
↓ Less than 1% | ↓ 11% |
| Colestipol 10 mg BID, 28 weeks |
40 mg QD for 28 weeks |
Not determined |
↓ 26%§ |
| Maalox TC® 30 mL QD, 17 days | 10 mg QD for 15 days |
↓ 33% | ↓ 34% |
| Efavirenz 600 mg QD, 14 days |
10 mg for 3 days |
↓ 41% | ↓ 1% |
| †Rifampin 600 mg QD, 7 days (co-administered) ¶ | 40 mg SD |
↑ 30% | ↑ 2.7-fold |
| †Rifampin 600 mg QD, 5 days (doses separated) ¶ | 40 mg SD |
↓ 80% | ↓ 40% |
| †Gemfibrozil 600mg BID, 7 days | 40 mg SD |
↑ 35% | ↓ Less than 1% |
| †Fenofibrate 160mg QD, 7 days | 40 mg SD |
↑ 3% | ↑ 2% |
Data given as x-fold change represent a simple ratio between co-administration and atorvastatin alone (i.e., 1-fold = no change). Data given as % change represent % difference relative to atorvastatin alone (i.e., 0% = no change).
†
See
WARNINGS, Skeletal Muscleand
PRECAUTIONS, Drug Interactionsfor clinical significance.
‡
Greater increases in AUC (up to 2.5-fold) and/or Cmax (up to 71%) have been reported with excessive grapefruit consumption (≥ 750 mL – 1.2 liters per day).
§
Single sample taken 8-16 h post dose.
¶
Due to the dual interaction mechanism of rifampin, simultaneous co-administration of atorvastatin with rifampin is recommended, as delayed administration of atorvastatin after administration of rifampin has been associated with a significant reduction in atorvastatin plasma concentrations.
How Supplied / Storage and Handling
CADUET tablets contain amlodipine besylate and atorvastatin calcium equivalent to amlodipine and atorvastatin in the dose strengths described below.
CADUET tablets are differentiated by tablet color/size and are engraved with "Pfizer" on one side and a unique number on the other side. CADUET tablets are supplied for oral administration in the following strengths and package configurations:
| CADUET | ||||
|---|---|---|---|---|
| Package Configuration |
Tablet Strength (amlodipine besylate/ atorvastatin calcium) mg |
NDC # | Engraving | Tablet Color |
|
|
|
|
|
|
| Bottle of 30 |
2.5/20 | 54868-5672-0 | CDT 252 | White |
| Bottle of 30 | 2.5/40 | 54868-5699-0 |
CDT 254 | White |
| Bottle of 30 Bottle of 90 |
5/10 | 54868-3287-0 54868-3287-1 |
CDT 051 | White |
| Bottle of 30 Bottle of 90 |
5/20 | 54868-1207-0 54868-1207-1 |
CDT 052 | White |
| Bottle of 30 | 5/40 | 54868-5179-0 | CDT 054 | White |
| Bottle of 30 | 5/80 | 54868-5420-0 |
CDT 058 | White |
| Bottle of 30 | 10/10 | 54868-5567-0 | CDT 101 | Blue |
| Bottle of 30 Bottle of 90 |
10/20 | 54868-5209-0 54868-5209-1 |
CDT 102 | Blue |
| Bottle of 30 Bottle of 90 |
10/40 | 54868-5200-0 54868-5200-1 |
CDT 104 | Blue |
| Bottle of 30 Bottle of 90 |
10/80 | 54868-5523-0 54868-5523-1 |
CDT 108 | Blue |
Store at 25°C (77°F); excursions permitted to 15–30°C (59–86°F) [see USP Controlled Room Temperature].
Rx only
Manufactured by:
Pfizer Ireland Pharmaceuticals
Dublin, Ireland

LAB-0276-15.0
January 2010
image of Pfizer logoPatient Counseling Information

Read the patient information that comes with CADUET before you start taking it, and each time you get a refill. There may be new information. This information does not replace talking with your doctor about your condition or treatment. If you have any questions about CADUET, ask your doctor or pharmacist.
What is CADUET?
CADUET is a prescription drug that combines Norvasc® (amlodipine besylate) and Lipitor® (atorvastatin calcium) in one pill.
CADUET is used in adults who need both Norvasc and Lipitor.
Norvasc is used to treat:
- High blood pressure (hypertension) and
- Chest pain (angina) and
- Blocked arteries of the heart (coronary artery disease)
Lipitor is used to lower the levels of "bad" cholesterol and triglycerides in your blood. It can also raise the levels of "good" cholesterol.
Lipitor is also used to lower the risk for heart attack, stroke, certain types of heart surgery, and chest pain in patients who have heart disease or risk factors for heart disease such as:
- age, smoking, high blood pressure, low HDL-C, heart disease in the family
Lipitor can lower the risk for heart attack or stroke in patients with diabetes and risk factors such as:
- diabetic eye or kidney problems, smoking, or high blood pressure.
CADUET has not been studied in children.
Who should not use CADUET?
Do not use CADUET if you:
- Are pregnant or think you may be pregnant, or are planning to become pregnant. CADUET may harm your unborn baby. If you get pregnant, stop taking CADUET and call your doctor right away.
- Are breastfeeding. CADUET can pass into your breast milk and may harm your baby. Do not breastfeed if you take CADUET.
- Have liver problems.
- Are allergic to anything in CADUET. The active ingredients are atorvastatin calcium and amlodipine besylate. See the end of this leaflet for a complete list of ingredients.
What should I tell my doctor before taking CADUET?
Tell your doctor about all of your health conditions, including, if you have:
- heart disease
- muscle aches or weakness
- diabetes
- thyroid problems
- kidney problems
- or drink more than 2 glasses of alcohol daily
Tell your doctor about all the medicines you take including prescription and nonprescription medicines, vitamins and herbal supplements. CADUET and some other medicines can interact, causing serious side effects. Especially tell your doctor if you take medicines for:
- your immune system
- infections
- cholesterol
- birth control
- heart failure
- HIV (AIDS)
You can use nitroglycerin and CADUET together. If you take nitroglycerin for chest pain (angina), do not stop taking it while taking CADUET.
Know all the medicines you take. Keep a list of them with you to show your doctor and pharmacist.
How should I take CADUET?
- Take CADUET once a day, exactly as your doctor tells you. Do not change your dose or stop CADUET without talking to your doctor.
- Take CADUET each day at any time of day, at about the same time each day. CADUET can be taken with or without food.
- Do not break the tablets before taking them. Talk to your doctor if you have a problem swallowing pills.
- Your doctor should start you on a low-fat diet before giving you CADUET. Stay on this low-fat diet when you take CADUET.
- CADUET comes in many different strengths. Your doctor will test your cholesterol and blood pressure to find the right dose for you.
- If you miss a dose, take it as soon as you remember. Do not take CADUET if it has been more than 12 hours since your missed dose. Just take the next dose at your regular time. Do not take 2 doses of CADUET at the same time.
- If too much CADUET is taken by accident, call your doctor or poison control center, or go to the nearest emergency room.
What should I avoid while taking CADUET?
- Avoid getting pregnant. If you get pregnant, stop taking CADUET right away and call your doctor.
- Do not breastfeed. CADUET can pass into your breast milk and may harm your baby.
What are possible side effects of CADUET?
CADUET can cause serious side effects. These side effects happen only to a small number of people. Your doctor can monitor you for them. These side effects usually go away if your dose is lowered or CADUET is stopped. These serious side effects include:
- Muscle problems. CADUET can cause serious muscle problems that can lead to kidney problems, including kidney failure. You have a higher chance for muscle problems if you are taking certain other medicines with CADUET.
- Liver problems. CADUET can cause liver problems. Your doctor may do blood tests to check your liver before you start taking CADUET and while you take it.
Call your doctor right away if:
- you have muscle problems like weakness, tenderness, or pain that happen without a good reason, especially if you also have a fever or feel more tired than usual
- allergic reactions including swelling of the face, lips, tongue, and/or throat that may cause difficulty in breathing or swallowing which may require treatment right away.
- you have nausea and vomiting, stomach pain
- you are passing brown or dark-colored urine
- you feel more tired than usual
- your skin and white of your eyes get yellow
- allergic skin reactions.
- Chest pain that does not go away or gets worse. Sometimes, when you start CADUET or increase your dose, chest pain can get worse or a heart attack can happen. If this happens, call your doctor or go to the emergency room right away.
Common side effects of CADUET include:
- headache
- tiredness
- stomach pain
- upset stomach
- swelling of your legs or ankles (edema)
- hot or warm feeling in your face (flushing)
- irregular heartbeat (arrhythmia)
- very fast heartbeat (heart palpitations)
- muscle and joint pain
- alterations in some laboratory blood tests
- dizziness
- extreme sleepiness
- nausea
- diarrhea
Additional side effects have been reported: tendon problems.
Talk to your doctor or pharmacist about side effects that bother you or do not go away.
There are other side effects of CADUET. Ask your doctor or pharmacist for a complete list.
How do I store CADUET?
- Store CADUET at room temperature, 68 to 77°F (20 to 25°C).
- Do not keep medicine that is out-of-date or that you no longer need.
- Keep CADUET and all medicines out of the reach of children. Keep medicines in places where children cannot get it.
General information about CADUET
Medicines are sometimes prescribed for conditions that are not mentioned in patient information leaflets. Do not use CADUET for a condition for which it was not prescribed. Do not give CADUET to other people, even if they have the same problem you have. It may harm them.
This leaflet summarizes the most important information about CADUET. If you want more information, talk with your doctor. Ask your doctor or pharmacist for information about CADUET written for health professionals. You can also go to the CADUET website at www.CADUET.com, or call 866-514-0900.
What is high blood pressure (hypertension)?
You have high blood pressure when the force of blood against the walls of your arteries stays high. This can damage your heart and other parts of your body. Drugs that lower blood pressure lower your risk of having a stroke or heart attack.
What is angina (chest pain)?
Angina is a pain that keeps coming back when part of your heart does not get enough blood. It feels like something is pressing or squeezing your chest under the breastbone. Sometimes you can feel it in your shoulders, arms, neck, jaw, or back.
What is cholesterol?
Cholesterol is a fat-like substance made in your body. It is also found in foods. You need some cholesterol for good health, but too much is not good for you. Cholesterol can clog your blood vessels.
What is a heart attack?
A heart attack occurs when heart muscle does not get enough blood. Symptoms include chest pain, trouble breathing, nausea, and weakness. Heart muscle cells may be damaged or die. The heart cannot pump well or may stop beating.
What is a stroke?
A stroke occurs when nerve cells in the brain do not get enough blood. The cells may be damaged or die. The damaged cells may cause weakness or problems speaking or thinking.
WHAT ARE THE INGREDIENTS IN CADUET?
Active ingredients: amlodipine besylate, atorvastatin calcium
Inactive ingredients: calcium carbonate, croscarmellose sodium, microcrystalline cellulose, pregelatinized starch, polysorbate 80, hydroxypropyl cellulose, purified water, colloidal silicon dioxide (anhydrous), magnesium stearate
Film coating: Opadry® II White 85F28751 (polyvinyl alcohol, titanium dioxide, PEG 3000 and talc) or Opadry® II Blue 85F10919 (polyvinyl alcohol, titanium dioxide, PEG 3000, talc, and FD&C blue #2)
Rx only
Manufactured by Pfizer Ireland Pharmaceuticals
Dublin, Ireland

LAB-0347-3.0
July 2009